- Symptoms and recovery signals can worsen before the hospital knows.
- Delayed escalation increases avoidable complications and readmission risk.
- Outcome visibility drops sharply once care leaves the facility.
The Missing Stage in Healthcare: Care Continuity
Hospitals manage admission, diagnosis, treatment, and discharge. But patient outcomes are determined after discharge.
Care Continuity Technology (CCT) gives hospitals visibility, governance, and intervention capability beyond the hospital walls.
Operationalise recovery, adherence, monitoring, and intervention — as a structured hospital program.
Hospitals lose visibility after discharge
Hospitals invest heavily in clinical excellence inside the facility. But the most critical phase of recovery begins after the patient leaves the hospital. During this stage, follow-ups are missed, medication adherence drops, warning signals go unnoticed, and complications escalate late.
- Calls, WhatsApp, spreadsheets, and manual follow-up create coordination overhead.
- Triage and escalation remain inconsistent without structured workflows.
- Documentation gaps weaken accountability and auditability.
- Downstream services leak to external players without a hospital continuity layer.
- Hospitals miss recurring revenue tied to structured recovery programs.
- Unmeasured ROI makes scale decisions slower and less confident.
What is Care Continuum Technology (CCT)?
Healthcare has historically operated through four stages: admission, diagnosis, treatment, and discharge. But modern outcomes increasingly depend on the Fifth stage — Care Continuity.
What this stage includes
- Adherence monitoring across medicines, activities, and care instructions
- Symptom and vitals tracking during the vulnerable recovery window
- Milestone progression for protocol-driven programs
- Escalation and intervention when recovery deviates from expected pathways
How is CCT structured?
Three engines of care, powered by a platform layer - for governance, engagement, commerce, workflows, and analytics.

How does CCT execute care?
CCT focuses on the three execution models that EMRs don’t run — programs, services, and monitoring.
PROGRAM-DRIVEN CARE
- Executable care packages built on clinical pathways
- Automated follow-ups, adherence tracking, and engagement
- Defined triage, escalations, and closure criteria
- Outcomes and program performance reporting
SERVICE-DRIVEN CARE
- Hospital-controlled ordering and fulfilment
- Lab, pharmacy, nurse/doctor, therapy, equipment — one workflow
- Geo-tracking, SLAs, proof-of-service and patient feedback
- Integrated payments: packages, subscriptions, pay-per-service
SIGNAL-DRIVEN CARE
- Vitals, symptoms, milestones, recovery signals captured continuously
- Alerts converted into governed triage decisions
- Interventions, escalations, and longitudinal outcomes
- Dashboards across operational, clinical and financial performance
How it works — in 4 steps
A governed continuity loop that scales without scaling clinician workload.
Two Apps. One Governance Layer.
Experience layer designed for protocol execution, triage efficiency, and leadership visibility.
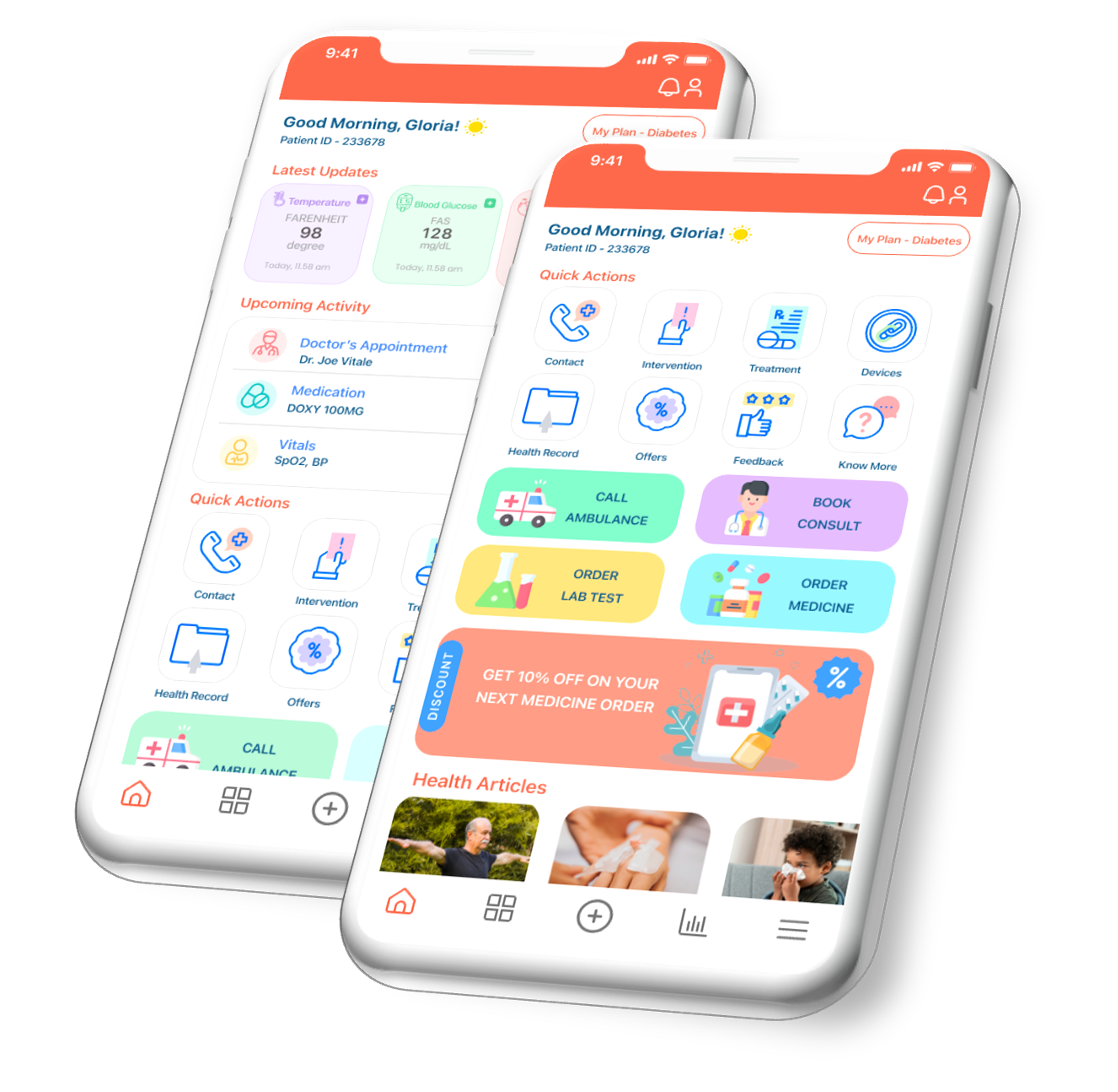
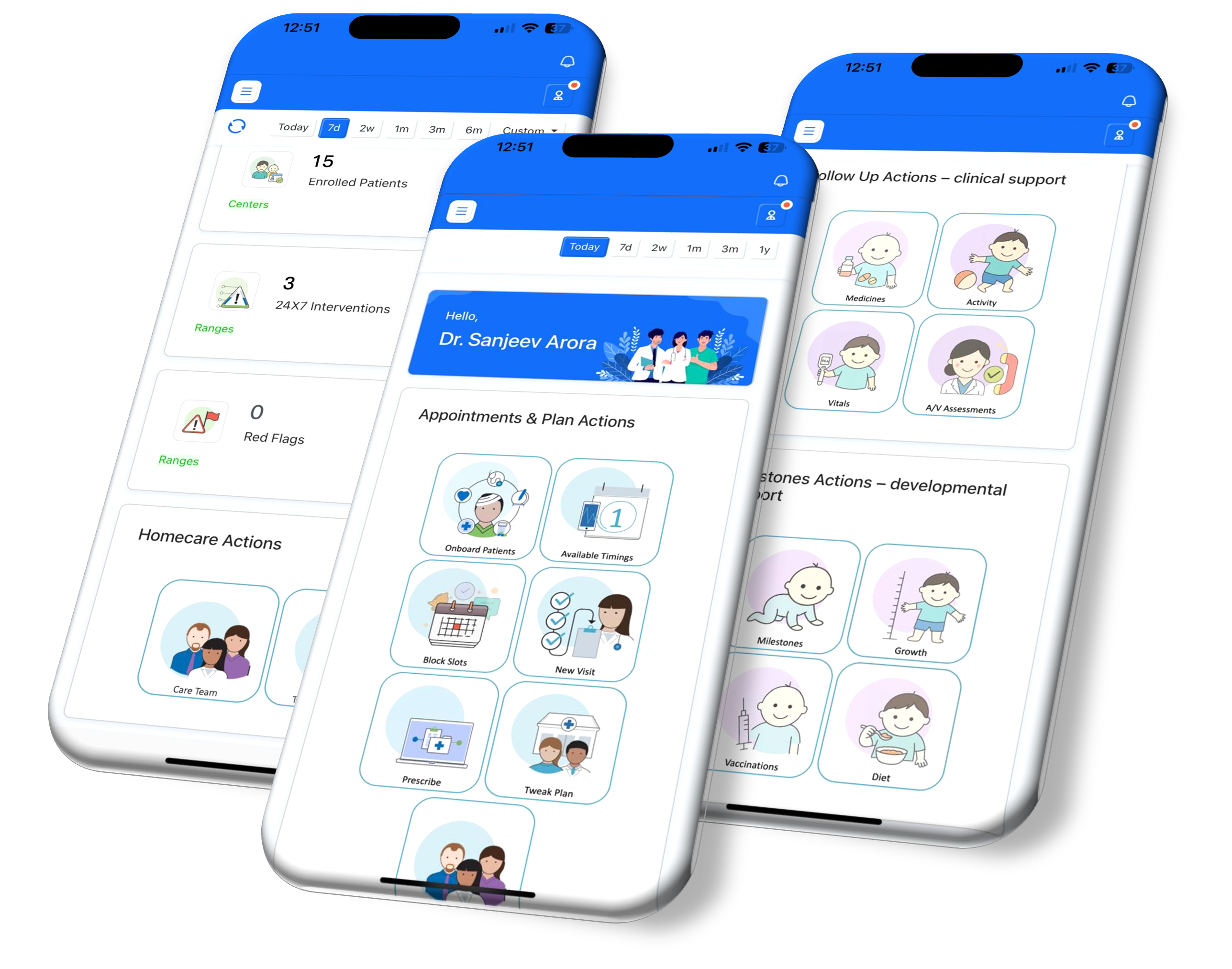
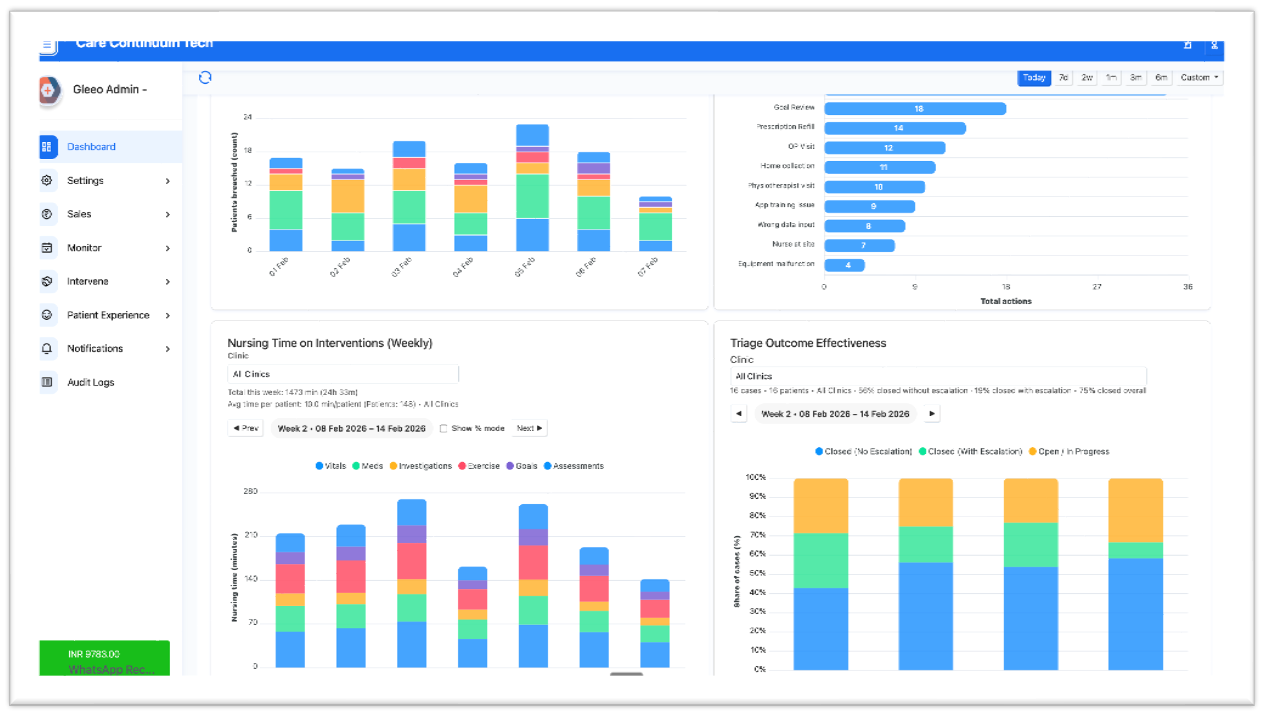
Intelligence, governance & trust
Distributed care requires control. CCT provides dashboards, audit trails, and outcomes visibility so hospitals govern continuity confidently.
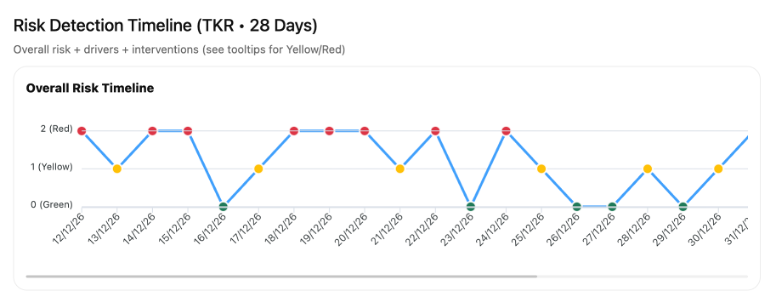
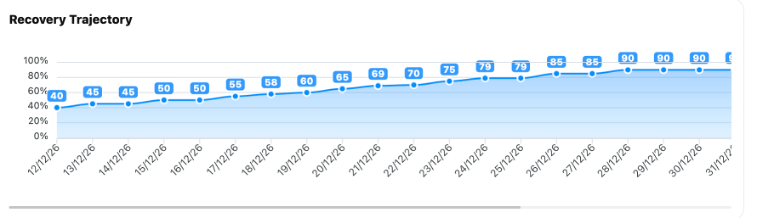
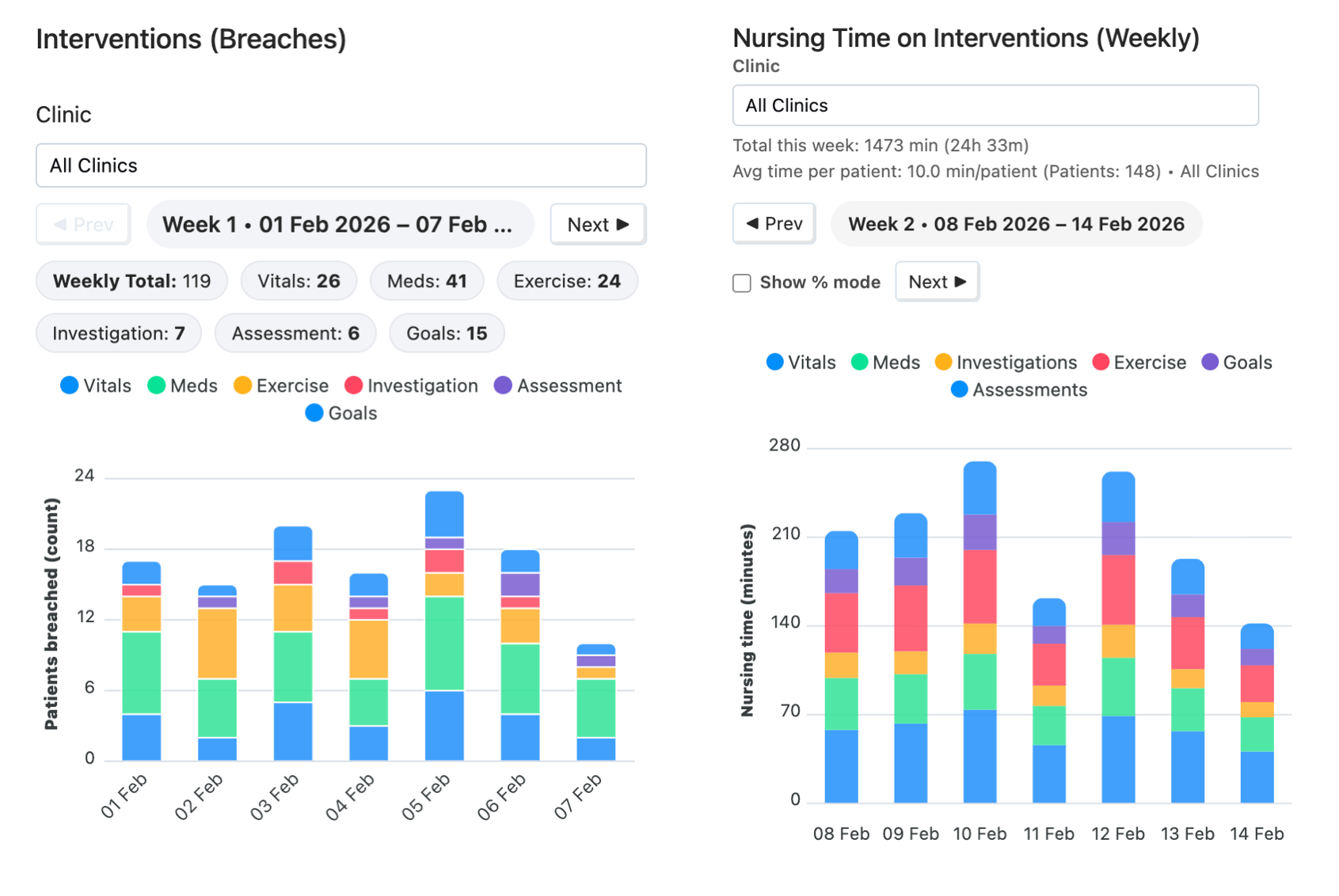
Measured outcomes, not promises
Hospital-controlled monitoring, early risk detection, measurable recovery, and protocol compliance.
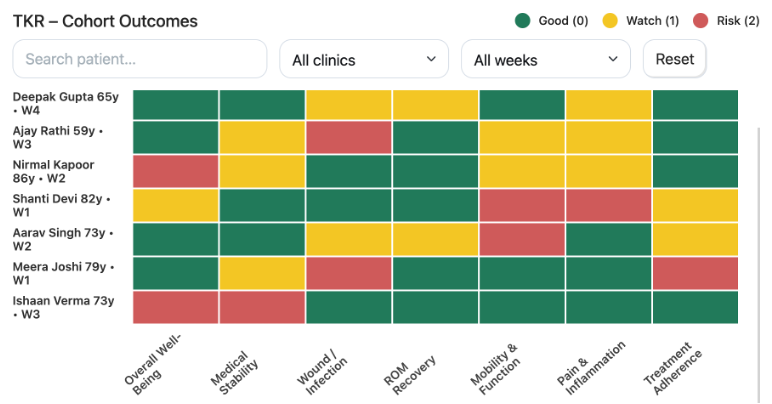
Interoperability: integrates on top of your systems
Integrates on top of HIS, EMR, LIS, and billing systems to enable continuity without rip-and-replace.
- Patient demographics and identifiers
- Discharge summaries and clinical context
- Billing-led enrollment triggers (packages/programs)
- Prescriptions for enrolled cohorts
- Lab results for enrolled cohorts
- Program summaries back to hospital record
Your HIS/EMR remains the system of record. CCT becomes the continuity engine orchestrating pathways, fulfilment, triage, interventions, and outcomes.
Compliance & data protection
Built for hospital-grade governance with role-based access, audit trails, secure workflows, and privacy-ready controls.
Where hospitals deploy CCT first
Start where post-acute risk, follow-up volume, and downstream demand are highest — then scale across specialties.

Engagement options: start small, scale fast
A structured approach that fits hospital procurement, operations, and clinical governance.
- 4–8 week focused rollout
- Packaged care automation + triage desk
- Scoped integration touchpoints
- Outcome baseline and reporting
- Operationalise on-demand fulfilment
- SLA dashboards + visit verification
- Escalation governance and audits
- Revenue tracking per program
- Packaged care + fulfilment + Continuous monitoring
- Full governance + longitudinal outcomes
- Interoperability framework across systems
- Expansion playbook across cohorts
IP & differentiation
Our patented infrastructure anchors the packaged care engine and signal-to-intervention workflows — with Continuous Monitoring as a natural extension of the same core.
Recognition & credibility
Signals that matter to hospital leadership and partners.




- Forbes – Most Valuable Companies (2025)
- Outlook India – 10 Visionary Leaders Shaping India’s Tomorrow (2026)
- Businessworld – 30 Under 30 (2024)
- Top 10 Healthcare CEOs (2023)
- Dubai BTX Asia's Top 10 Women Entrepreneur Awards (2023)
FAQ
Short answers to the questions hospital leaders ask first.
About Gleeo Health & leadership
Built by healthcare and technology leaders focused on a global gap hospitals face: continuity beyond four walls.
We enable hospitals and care teams to extend hospital-level care into homes through a governed technology layer. CCT turns packaged care, on-demand fulfilment, and chronic monitoring into measurable programs with outcomes visibility.
Hospitals do exceptional work inside their facilities — but outcomes are decided across the full patient journey. We built CCT so care beyond discharge is not informal or external, but hospital-controlled and accountable. Our goal is simple: make continuity executable, measurable, and scalable — globally.
Leadership with deep experience across healthcare delivery, enterprise healthtech, and care continuum programs. We work closely with hospital CEOs, CMOs, CIOs and operations leaders to make continuity sustainable and revenue-positive.
Schedule an executive discussion
Share your specialty focus and goals. We’ll propose a rollout model, integration approach, and governance plan.



